The integration of AI into surgical robots could radically change the way operations are performed. According to researchers at King’s College London, the future of surgery lies in so-called ‘embodied AI’: robots that not only perform tasks but also learn, analyse and provide support during surgery. In a recent publication, they outline how this development could lead to ‘truly personalised surgery’, provided that key ethical and regulatory issues are resolved.
The researchers emphasise that AI-driven robots have the potential to improve the performance of surgical teams, but that this can only be done safely under strict human and institutional control. The analysis was recently published in Frontiers in Science.
A new generation of surgery
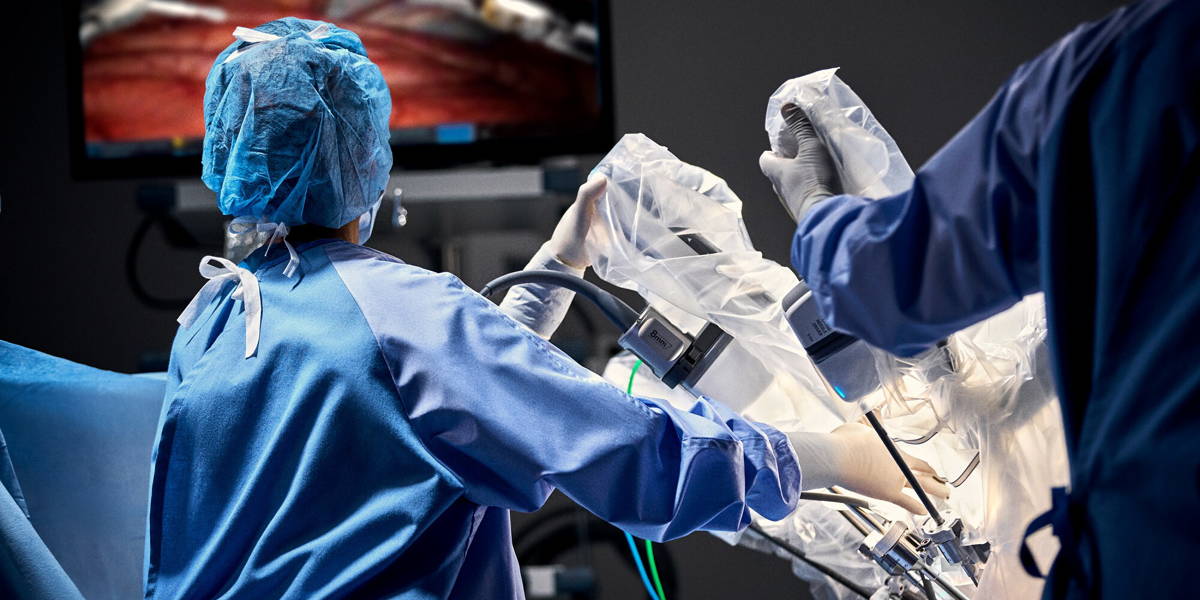
Surgical robots have long been part of the operating room, but until now have primarily functioned as advanced instruments controlled entirely by the surgeon. With the advent of AI, that foundation is changing. By integrating artificial intelligence directly into robotic systems, a new generation of technology is emerging that can learn from data, adapt to circumstances and provide real-time support.
This ‘embodied AI’ is linked to sensors in the operating room that continuously collect data on the patient, the environment and the team’s actions. This creates a dynamic system that develops spatial awareness and can analyse and optimise surgical procedures.
According to lead researcher Prokar Dasgupta, this development will influence all phases of surgery: from technique and workflow to decision-making and collaboration within teams. Robots can, for example, assist in emergency situations, provide support during complex procedures and offer feedback during the operation.
Real-time personalised care
One of the most promising applications is AI’s ability to personalise operations. By combining large amounts of patient data with real-time information from the operating room, systems can support surgeons in choosing the best possible treatment for a specific patient.
Future AI systems will be able to simulate different scenarios and predict the expected outcomes of potential procedures. This so-called cause-and-effect insight makes it possible to better substantiate decisions before an action is actually carried out.
According to Alejandro Granados, surgery is thus on the cusp of a fundamental transformation. Technology will not only support but actively guide treatment choices, with the aim of achieving better outcomes and fewer complications for patients.
Regulation of learning systems
However, the emergence of AI-driven robots also raises new questions about safety and regulation. Traditionally, medical technologies are approved on the basis of a fixed configuration. AI systems that continue to learn and adapt after being introduced into clinical practice do not fit within that model.
The researchers therefore advocate for changes to regulations, including new authorisation procedures, stricter post-market monitoring and revised classifications for medical devices. There is also a need for standardised methods to evaluate the performance of AI and the interaction between humans and machines.
In addition, attention must be paid to bias in datasets, which can exacerbate existing inequalities in healthcare. As much research and development takes place in affluent countries, there is a risk that other regions will benefit less from these innovations.
Changing role of the healthcare team
As the autonomy of robotic systems increases, the role of the surgeon and the surgical team is also changing. It is expected that surgeons will focus more on supervision and strategic decision-making, whilst support staff develop new skills in technology and data.
At the same time, new roles are emerging within the team, such as clinical data specialists and engineers responsible for integrating AI and robotics into practice. Despite this shift, one principle remains central: humans remain in control.
The researchers emphasise that surgeons must retain ultimate responsibility for decisions during operations. AI should provide support, not be a replacement. Clear communication and a clear division of roles within the team are essential for safe care.
Crucial implementation
Although the potential of AI-driven surgery is vast, the authors stress that careful implementation is crucial. New models of collaboration between academic institutions, industry and healthcare organisations are needed to develop the technology responsibly and make it accessible. Furthermore, global application requires attention to affordability and equal access, so that countries with fewer resources can also benefit from these developments.
The coming years will be decisive for how AI and robotics develop in the operating room. If technological progress goes hand in hand with robust regulation and human oversight, this could lead to safer, more accurate and more personalised care. The operating room of the future will thus become not only smarter, but also more adaptive, with technology that learns, but people who remain in control.
AI co-pilot for surgeons
During the Surgical AI & Telesurgery Days in Ghent in February this year, Orsi Academy presented an AI co-pilot that supports surgeons in real time during robotic surgery. The system analyses live surgical images, recognises surgical phases and detects critical anatomical structures, contributing to greater precision and patient safety.
The technology builds on earlier innovations in which multiple AI models were deployed simultaneously, including for organ recognition and augmented reality during operations. With this new step, the focus shifts from experimentation to broader clinical application, across the entire surgical process. Thanks to the use of powerful supercomputing, the AI can function without delay. This development positions Belgium as a frontrunner in AI-driven surgery, but also raises questions regarding validation, regulation and implementation.