Natasha Azzopardi Muscat, Director of the Division of Health Systems at World Health Organization Regional Office for Europe, explains why trust, regulation, and equity will define the next phase of healthcare transformation, and why technology alone will not solve systemic challenges without the right policies, funding models, and workforce support.
WHO Europe regularly publishes reports and recommendations on digital health, including the recent "Building Financing Pathways for Digital Health Technologies in the WHO European Region." What impact does WHO Europe have in shaping effective health policies?
WHO/Europe was the first WHO Region to adopt a digital health strategy for the region as a whole. We did this in 2022 based on a comprehensive assessment across all 53 Member States. That gave us a clear roadmap to generate evidence, build country capacity, strengthen partnerships, and anticipate future trends, especially around AI.
Since then, and in line with the strategy, we have supported countries through the development of a series of technical, evidence-based publications on key issues, including supporting the uptake of digital solutions by the health and care workforce and finding smart ways to fund digital health effectively.
We’ve provided remote and in-person training and developed new forms of collaboration, including engagement with industry through our Strategic Partners Initiative for Data and Digital Health. We set up the Initiative to bring together all countries in our Region and leading partners in the fields of data and digital health. Digital health and AI have become key to how countries are rethinking their systems after COVID-19, particularly in the context of workforce shortages and rising demand.
But one message is clear: this transformation must be built on trust. AI has a role to play, but it must be ethical and well-regulated to ensure affordability and equitable access. It must also be evidence-based and deliver real value. It should support health workers – never replace them – while improving quality of care, at the same time remaining affordable for systems under financial pressure.
How would you assess the state of multilateralism in health in Europe today?
It’s clear that there are widening fractures in the traditional multilateral system, and we should not deny this but seek new ways in which to promote collaboration and collective approaches to global problems. But I don’t see it as all doom and gloom. In fact, I believe that multilateralism remains strong in Europe. Let’s not forget that many countries in Europe are small or medium-sized and thus rely on multilateral cooperation heavily to address shared challenges.
Obviously, the global environment is fraught, but I do believe that, in the main, Europe remains committed to multilateralism. So while we are seeing pressure on global institutions and growing skepticism, I think the real question is not whether multilateralism survives, but how it evolves. And across Europe, I do think many countries are leading this charge by actively exploring and investing in new forms of collaboration, such as through subregional networks, joint initiatives, and collective advocacy. Many also continue to play a strong role globally, as funders and champions of science and public health.
Will this be enough? Let’s say that I remain cautiously optimistic and that I do sense a clear commitment to adapt multilateralism to today’s realities.
In recent years, we have experienced accelerated digitalization in healthcare. Are there specific countries or use cases you cite as a blueprint?
Rather than highlighting individual countries or specific examples, we have documented a wide range of concrete use cases in our recent report “Artificial intelligence is reshaping health systems: state of readiness across the WHO European Region”.
These include applications in workforce optimization, early detection of noncommunicable diseases, and health system planning. The report provides practical examples that countries can adapt to their own contexts, grounded in real-world implementation.
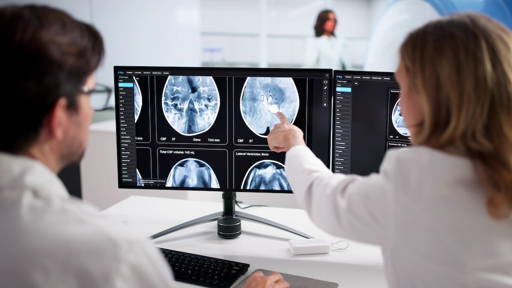
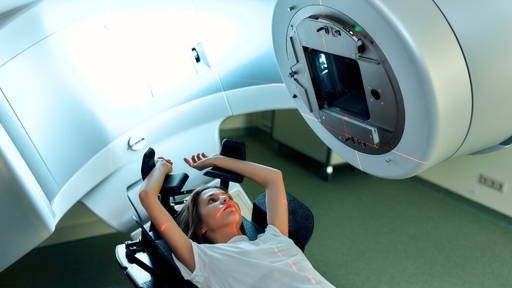
Of course, we’re all aware of the promise that AI holds in areas such as radiology, screening, telemedicine, and robotics, and there are recent ground-breaking examples from countries within the Region. But scalability is a key issue in this area. So while we should – and we do – encourage countries to share and learn from one another’s experiences, providing specific examples as ‘models’ may not necessarily be the best approach.
WHO has long advocated for equal access to healthcare. Digital health can help break existing barriers, for example, through telehealth services. At the same time, digital literacy and access to technology have become new determinants of health. How can digitalization be regulated to ensure it benefits everyone?
In my view, there is a clear paradox: those who could benefit the most from digital health tools are often the ones least able to access them.
We see this with older populations, those with learning and educational difficulties, people in rural areas, and underserved communities. While telemedicine and remote care have expanded access, especially since COVID-19, basic infrastructure gaps, including access to stable electricity, still exist in some settings.
We are therefore dealing with two realities at once: rapid innovation on one side, and persistent inequities on the other.
The solution lies in smart regulation and investment, specifically towards ensuring infrastructure, building digital literacy, and strengthening trust. Importantly, this is not only about patients. Health workers also need the skills and confidence to use these tools effectively, and we are working with our Member States, and with partners, to adapt teaching and training curricula and to ensure that our health and care workforce is equipped for current and indeed future challenges and opportunities.
But it’s equally important that people become more digitally literate – this will help ensure greater equality and that digital solutions deliver on their promises. Some of the most promising approaches bring communities together. For example, we see some countries having digital literacy education already in primary school. And this then translates into intergenerational learning, where these same young people can help or teach older family members how to navigate digital tools.
At the end of the day, digital health must remain human-centered. And I feel that we don’t repeat this often enough.
We are seeing a strong trend toward longevity. Is this a signal that prevention strategies must be rethought to become more attractive in the era of wearables and AI?
I would say that prevention is evolving, but the fundamentals remain the same.
As public health professionals, we have often made the mistake of choosing individual strategies rather than realizing that we need to be doing a little bit of everything.
Without question, digital tools such as wearables can support personalized prevention through data and feedback. But they must be complemented by strong public policies on environment, regulation, and the wider determinants of health. We need both.
I would also suggest that we need to recognize that digital and AI are now a commercial determinant of health in its own right. These represent goods we use daily that can have both positive and negative impacts on our health. Like food systems, they are essential but require careful regulation.
Finally, and overlapping with the earlier question, we must avoid creating a two-tier system where only those who are younger, more digitally literate, and who can afford personalized tools benefit from them. Equity and access must remain at the center of prevention strategies.
You have been working at WHO Europe for six years. What key developments, both positive and negative, have you observed during this time? And what kind of health system would you wish for the next generation?
These have been an intense but rewarding six years. I won’t deny that, in part, they have also been tough. We have faced major crises, not least the COVID-19 pandemic, the war in Ukraine, as well as a major internal restructuring due to a changing financial situation. But have also witnessed the promise and benefits of rapid technological change and increasing out-of-the-box thinking.
What stands out for me is our ability as WHO to connect the dots: health systems today must integrate workforce challenges, digital transformation, financing, prevention, and emergency preparedness, and all at the same time. I have been strongly advocating for the need to look beyond the health sector alone for solutions. Whether it’s Health in All Strategies or intersectoral and all-of-government approaches, the point is that during my time at WHO, I can see that we are increasingly more inclusive. For example, we are bringing in the finance and employment sectors and engaging with them in key areas such as primary health care, the health and care workforce crisis, and mental health. So too have we been far better at involving civil society in a meaningful way. Our 2024 Framework for Resilient and Sustainable Health Systems, endorsed by all Member States, was developed in a spirit of co-creation and makes clear that this is key to health system transformation itself.
Looking ahead, I’m always glad to repeat the framework's vision statement as it makes the goal clear: people should be able to access the right care, in the right place, at the right time, by the right professional, without financial hardship. And I firmly believe that today we have the science, technology, and mindset to make this possible. The challenge is to design systems with the right incentives, the right balance of services, and a strong political commitment to equity. And I regard it as a privilege to work towards this mandate with my teams, and crucial partners such as civil society, the European Commission, and OECD.
Ultimately, this is about enabling people not just to live longer, but to live healthier, more productive, and more fulfilling lives.