A new diagnostic approach combining a blood test, a standardized questionnaire, and artificial intelligence may significantly improve early detection of leprosy, particularly in endemic regions such as Brazil. Researchers from the University of São Paulo report promising results in a study.
Leprosy remains a major public health challenge, with more than 200,000 new cases reported annually worldwide, according to the World Health Organization. Early diagnosis is critical but difficult, as initial symptoms are often subtle and conventional laboratory tests lack sensitivity in early-stage disease. “Many patients are only diagnosed once symptoms become more pronounced,” says researcher Filipe Lima. “This delays treatment and increases the risk of complications and transmission.”
Combining AI with improved biomarkers
The research team developed a dual screening strategy. The first component is a digital clinical questionnaire, the Leprosy Suspicion Questionnaire (LSQ), enhanced with an AI tool (MaLeSQs) to identify early neurological symptoms.
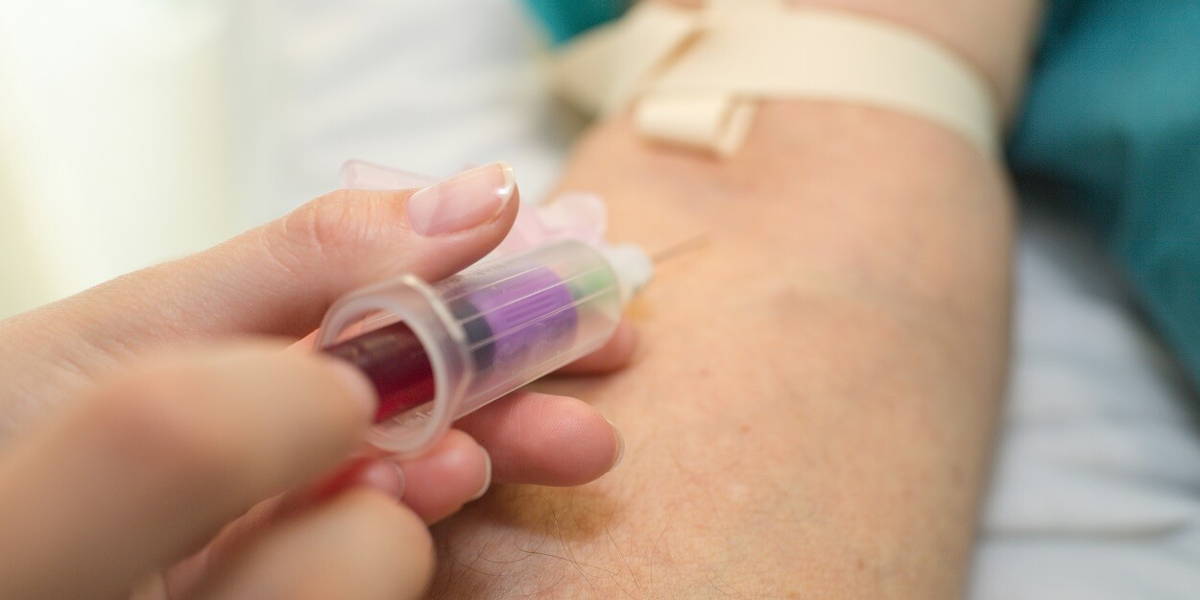
The second component is a blood test targeting the Mce1A antigen of Mycobacterium leprae. Unlike traditional tests that focus on a single antibody (PGL-I), the new assay detects multiple antibody classes (IgA, IgM, and IgG), improving sensitivity and enabling differentiation between exposure and active infection. The study was published in BMC Infectious Diseases.
Promising results
The method was evaluated using blood samples collected during a COVID-19 population study in Ribeirão Preto. Of 224 participants who completed the questionnaire, 195 underwent blood testing and 37 attended follow-up clinical evaluations.
The combined approach identified 12 previously undiagnosed leprosy cases, around one-third of those clinically assessed. Notably, these individuals had not reported clear symptoms prior to screening.
The IgM-based Mce1A test proved particularly effective, detecting two-thirds of confirmed cases. When combined with the AI-supported questionnaire, the system achieved 100% sensitivity in identifying suspected cases later confirmed by specialists.
Scalable and low-cost screening tool
Importantly, the new diagnostic approach is designed for scalability. The laboratory techniques required are comparable in cost and complexity to existing tests, making implementation feasible in routine clinical settings. “The test does not replace clinical diagnosis, but it helps identify who should be referred for specialist evaluation,” Lima explains. This could strengthen screening strategies within public health systems such as Brazil’s Sistema Único de Saúde.
The study also incorporated geospatial analysis, suggesting that leprosy exposure is more diffusely distributed than previously assumed, affecting diverse socioeconomic groups. Researchers are now working on further refining the biomarker to improve specificity and support large-scale validation. If successful, the approach could be integrated into national screening programs.
The findings highlight how combining AI with accessible diagnostics can address longstanding gaps in infectious disease detection, offering a pathway toward earlier intervention and improved disease control.
AI enhanced blood test
Last year, researchers from the University of Vienna and Nankai University showed that a simple blood test may reveal how well we are aging. By combining metabolomics, machine learning, and network modeling, they found a strong link between blood chemistry and physical fitness in older adults.
Using a Body Activity Index (BAI) and a metabolomics profile of 35 molecules, the study demonstrated a high correlation between physical performance and blood markers. AI models were able to distinguish active from less-active individuals with over 91% accuracy. Eight metabolites were identified as key predictors, with aspartate emerging as the strongest biomarker.