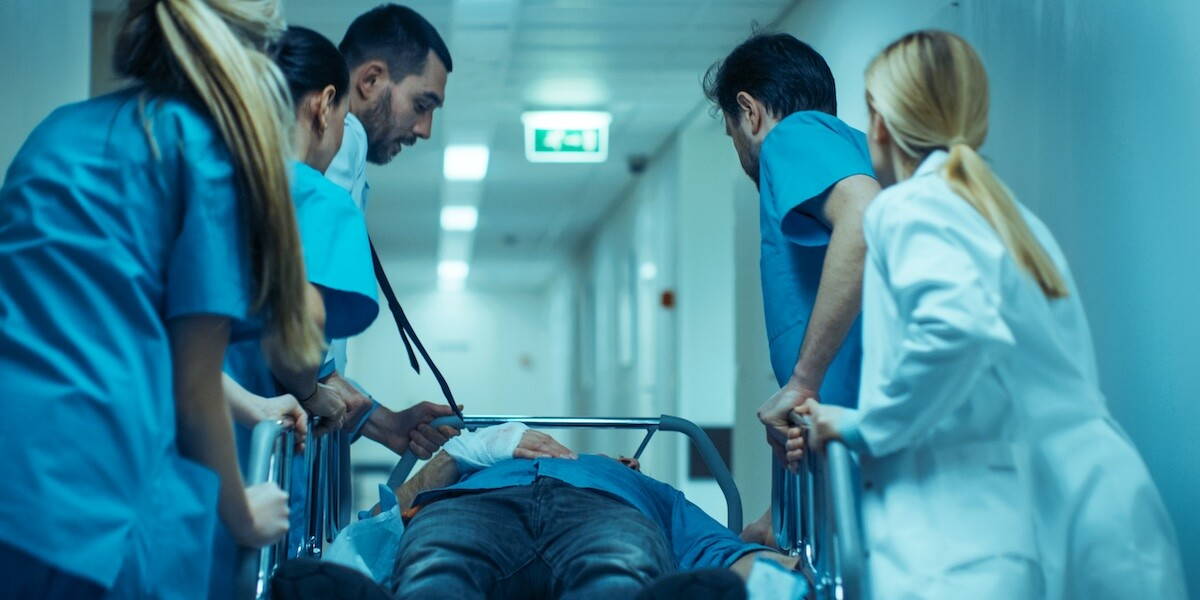
In an emergency room, a language gap can delay triage, blur consent and introduce risk at the exact moment decisions need to be made clearly and fast. If the goal is to achieve successful 24/7 interpreter support, a system that connects seamlessly, holds up under pressure and fits into the realities of emergency care is necessary.
Why 24/7 Interpretation Matters
Emergency departments expose every weakness in a language access plan. There are short decision windows, incomplete histories and handoffs that happen fast. If that stalls for any reason, the clinical risk escalates rapidly. That is why interpreter access in the emergency room should be considered as critical as triage flow, patient safety and throughput.
Federal guidance in the U.S. still treats meaningful access for people with limited English proficiency as a legal and operational obligation rather than an optional service layer. It is part of clinical governance that affects informed consent and diagnostic accuracy and whether discharge instructions are followed.
The American Academy of Emergency Medicine’s best-practice guide says family and friends should not serve as interpreters and recommends in-person, telephone and video interpreting as the appropriate service options. There should also be translated discharge materials available as part of the safety net.
Kristin Quinlan, the CEO of Certified Languages International (CLI)l, a provider that offers 24/7 access to trained interpreters, explains that “...the United States doesn’t have a national language of origin” and explains her beliefs that “...it’s considered a basic human right to have a provision of language access for people with limited English proficiency.”
The challenge lies not in deciding whether an emergency room needs 24/7 language access, but how to build a language model that connects quickly enough for urgent care, covers enough languages to be credible and still works for staff who have seconds rather than minutes to figure out the tool.
What the Best 24/7 Model Looks Like
In practice, the strongest model is usually layered. For most emergency departments, that means immediate phone access for the fastest connection, video remote interpreting when visual communication is necessary, and in-person support for cases that are prolonged, highly sensitive or clinically dense. While in-person interpreters are ideal, telephone and video services offer a more readily available and cost-effective route to access.
This is where on-demand interpreting services for emergency departments prove their value, especially during overnight shifts and patient surges. Phone interpreting is a fast way to conduct triage, take bedside history and provide basic updates. That's important when the issue is pain level, allergy confirmation or whether a patient took anticoagulants before arrival.
Video remote interpreting becomes more useful when a visual demonstration is more effective than a verbal explanation. Consider, for example, stroke assessment, informed consent, labor and delivery triage, mental health evaluations, or discharge teaching where facial cues and visual trust matter.
This model also helps with rare languages. Instead of trying to staff every language on-site around the clock, you can reserve scarce in-person resources for the cases that truly need them and rely on broader on-demand networks for the rest.
Operational details matter here. Put the access point where the work happens, like the triage desk, resuscitation bay and the pediatric area. If workers need to hunt for a device or reset passwords, the system will fail under pressure. Set a connect-time target and track it. Then, test it during peak hours and overnight.
Failure Points ERs Should Avoid
HIPAA-compliant interpreter services for hospitals are essential. Certified Language International’s CEO explains that “statistics show that the language services industry is projected to grow between 6-7% between now and 2030,” illustrating how the need is anticipated to come more to the forefront of care. However, even well-funded, well-organized emergency departments can weaken language access through avoidable design mistakes.
The first is relying on family members, friends or untrained employees to interpret urgent clinical conversations. Professional interpreting is preferable in this situation because emergency discussions often involve consent, safety risks and sensitive details.
NHS England’s 2025 improvement framework describes familiar barriers here, including inconsistent access, weak staff awareness and poor recording of patients’ language needs. In practice, that means the service exists, but there is still a delay.
Some U.S. hospitals solve this by putting interpreter access where the work happens. Boston Medical Center Health System describes dual-handset phones in key departments and video remote interpreting via an iPad-on-a-pole setup for situations such as ASL. This real-world example perfectly illustrates what CLI's Kristin Quinlan calls being “device agnostic.”
Another blind spot is treating spoken interpretation as the entirety of the task. Emergency communication extends into written instructions, medication directions and follow-up information. The NHS has highlighted real cases where weak translation support contributed to delays and breakdowns in care, which is a useful reminder that accessible communication is a pathway issue rather than a single encounter issue.
Finally, full reliance on AI poses a downfall for quality care. While AI is beneficial in helping to automate tasks, Quinlan from CLI explains that “...it [AI] certainly cannot understand emotions and cultural subtleties such as pop culture references and the like. Only a human is capable of such intricacy.” Dismissing the need for human interaction and communication poses a potential failure point for the future of language interpretation in emergency rooms and hospitals.
No Longer Lost in Translation
To achieve safer emergency care, language access needs to function like core infrastructure. The most effective approach is layered with immediate on-demand access for speed, video when visual clarity is necessary and in-person support for complex cases. The ultimate measure of success is whether clinicians reach a qualified interpreter quickly, at any hour and without disrupting the workflow.