The use of AI in European healthcare is growing rapidly, but the conditions for responsible implementation are lagging. This is evident from a new, comprehensive report by WHO/Europe, which for the first time provides a detailed overview of AI applications across all 27 member states of the European Union.
The report, prepared in collaboration with the European Commission, is based on data collected between June 2024 and March 2025. It reveals a sector that is actively experimenting and implementing AI, yet simultaneously grappling with strategic alignment, funding, and legislation. As a result, AI in healthcare is at a tipping point: the technology is ready for scaling up, but the ecosystem is not.
Unevenly distributed growth
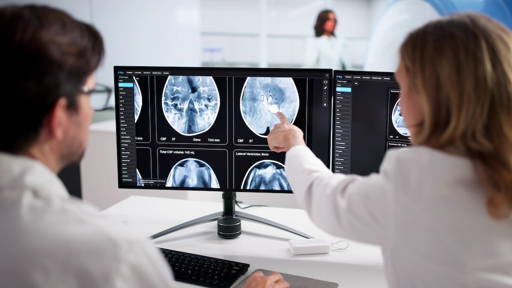
AI is beginning to noticeably transform healthcare systems across the EU. According to the report, the technology offers the prospect of more efficient service delivery, better patient outcomes, and relief from the pressure on overburdened healthcare professionals. In particular, AI-supported diagnostics are on the rise, as are chatbots that support patient engagement and self-management.
Nevertheless, adoption is unevenly distributed. Although many member states have identified priority areas of application, fewer than two-thirds have actually allocated specific funding for development, testing, and implementation. The high initial costs for technology, infrastructure, and training pose a significant barrier, especially for countries with limited resources.
In addition, structural barriers play a role. Member states cite financial feasibility, legal uncertainty, and inadequate data quality and standards as the main obstacles. Without targeted investments, there is a risk of a divide emerging between countries that can quickly integrate AI and those that lag.
Strategy and practice do not align
Progress is visible at the policy level, but coherence is often lacking. Most EU countries have national AI strategies, but these are typically cross-sectoral and not specifically tailored to healthcare. Only a few Member States have developed a separate health strategy for AI or are in the process of doing so.
According to WHO/Europe, this poses a risk. While broad strategies offer consistency, they do not always align with the specific needs of healthcare systems. The report therefore advocates for better alignment between general AI policy frameworks and national health goals.
Governance and the division of responsibilities are also still evolving. In many countries, there is no clear designation of the parties responsible for implementing and monitoring AI strategies. This hinders effective coordination and can lead to fragmentation.
Trust and legislation under pressure
One of the most urgent bottlenecks is the limited capacity of the healthcare labor market. Fewer than half of the member states have created new positions for AI and data expertise in healthcare, and training opportunities remain scarce. This is even though healthcare professionals remain responsible for decisions in which AI plays a role.
In addition, stakeholder engagement appears to be insufficiently broad. Consultations focus primarily on governments, healthcare institutions, and academic parties, while patients and citizens are involved less frequently. According to the report, this can lead to solutions that are insufficiently aligned with practice, receive less public support, or even exacerbate existing health disparities.
The landscape remains fragmented in legal and ethical terms as well. Although many countries are working to identify legal gaps, specific AI regulations for healthcare are still rare. Post-market monitoring of AI applications is limited, and liability issues are often unclear.
The report emphasizes that robust and harmonized regulations are essential to ensure patient safety and support innovation. This also includes greater focus on transparency, risk assessment, continuous monitoring, and clear responsibilities for developers, healthcare providers, and institutions.
At the same time, the European Commission highlights the importance of European initiatives such as the European Health Data Space (EHDS), which is set to play a crucial role in data sharing and the development of AI applications starting in 2029. Close alignment with existing regulations, such as the GDPR, is essential in this regard.
Balance between innovation and safeguards
Despite the challenges, the direction is clear: AI will play an increasingly central role in European healthcare. The technology offers concrete opportunities to make care more accessible, efficient, and patient-centered.
However, to fulfill that promise, a comprehensive approach is needed. The report advocates for a combination of targeted investments, skills development, inclusive policymaking, and sustainable financing models. Establishing centers of expertise and European platforms for validated AI solutions can also contribute to safe and equitable implementation.
The core message of the WHO/Europe report is thus clear: technological progress alone is not enough. Without strong governance, broad public support, and well-trained professionals, AI in healthcare risks failing to fully realize its potential. The coming years will be decisive in determining whether Europe succeeds in striking this balance.