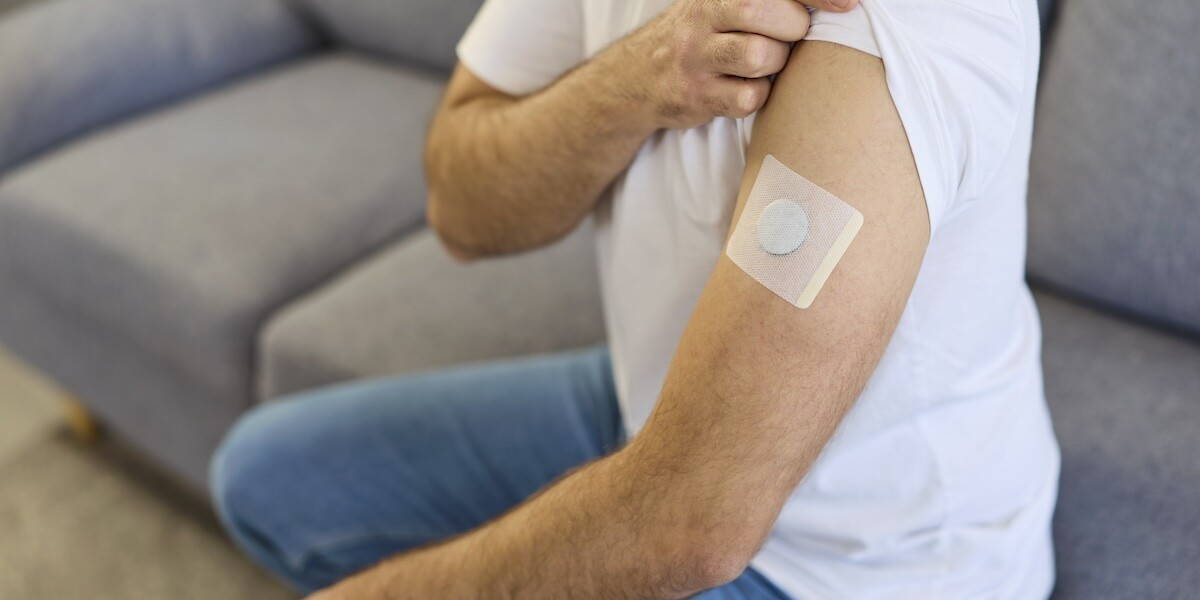
Diabetic foot ulcers remain one of the most serious complications of diabetes, often leading to infection, tissue damage and, in severe cases, amputation. Early detection is critical, yet continuous monitoring is difficult in daily practice. Now, researchers have developed a smart wound dressing that could significantly improve how these ulcers are managed.
The innovation is a wireless, battery-free patch that enables real-time monitoring of wound conditions. By combining advanced materials with digital sensing, the technology aims to detect complications earlier and reduce the risk of severe outcomes.
Multi-sensor patch
The smart patch integrates an optoelectronic sensor with a functional wound dressing. It can simultaneously measure key indicators of wound health, including glucose levels, pH (acidity) and temperature. These parameters are closely linked to infection and tissue deterioration in diabetic ulcers.
Patients can access this information directly via a smartphone, allowing for continuous self-monitoring outside clinical settings. This shift towards real-time, at-home monitoring could help bridge the gap between hospital visits and enable faster clinical intervention when needed.
Early warning
A distinctive feature of the patch is its nanofiber-based dressing, developed using electrospinning techniques. The material changes color in response to biochemical changes in the wound environment, such as rising glucose levels or shifts in acidity.
This visual feedback provides an intuitive early warning system: worsening wound conditions can be detected at a glance, without the need for specialised equipment. Importantly, the approach is non-invasive, eliminating the need for repeated blood sampling or tissue extraction.
The research was led by Inkyu Park in collaboration with international partners, including California Institute of Technology and Hanbat National University.
Battery-free design
To enhance diagnostic accuracy, the patch incorporates an optoelectronic system consisting of a light-emitting diode and a photodiode. These components measure changes in the dressing’s colour as light reflectance and convert them into electrical signals, providing more stable data than camera-based methods.
A key innovation is the use of near-field communication (NFC), which allows the patch to operate without a battery. When a smartphone is placed near the patch, it wirelessly supplies power and retrieves the data. This simplifies usage and removes the need for bulky or complex equipment.
Both patients and healthcare professionals can therefore monitor wound status in real time using a dedicated app, supporting timely and informed decision-making.
Promising technology
The combination of visual cues and quantitative data makes the technology particularly promising for clinical use. By enabling continuous, non-invasive monitoring, the patch could reduce the need for frequent hospital visits and improve patients’ quality of life.
According to Park, the research originated from the goal of reducing the burden of daily finger-prick tests for people with diabetes. The resulting platform may extend beyond wound care, offering potential for broader, blood-free diagnostic applications in chronic disease management.
While further validation and clinical testing are needed, the development highlights the growing role of smart wearables in healthcare. For the ICT&health sector, it represents another step towards integrated, patient-centred care, where digital technologies support early diagnosis, continuous monitoring and more personalised treatment pathways.
Monitoring patch
Last month we wrote about another smart wound dressing, developed by researchers at RMIT University that can both monitor wound conditions and automatically deliver treatment. The innovation targets chronic wounds, which require intensive, long-term care and place a significant burden on healthcare systems.
The dressing integrates carbon dots, multifunctional nanoparticles, into a hydrogel. These particles detect changes such as pH shifts linked to infection and respond by changing colour, which can be read via smart devices. At the same time, they act as nanozymes, automatically releasing therapeutic agents to reduce inflammation and promote healing. Treatment can also be manually activated by applying light pressure.